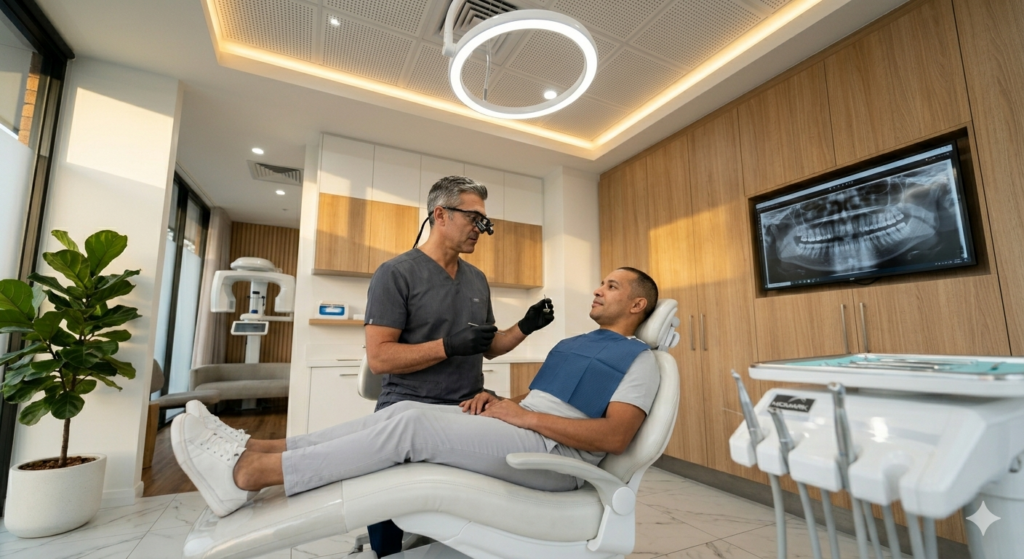
You face dental pain or a sudden injury, and you want clear, fast help in Burbank — not guesswork. If a tooth is knocked out, bleeding won’t stop, or pain spikes with swelling, seek emergency dental care right away to protect your smile and prevent complications.
This article guides you through the signs that demand urgent attention, what to do before you reach a dentist, and modern treatment options available in Burbank. It also explains how to choose a trustworthy emergency dentist, practical aftercare steps, and simple prevention tips so you can handle the crisis calmly and confidently.
Signs You Need Urgent Dental Care
Persistent, worsening, or suddenly severe tooth or gum problems often require same-day attention to prevent complications. Look for intense pain, uncontrolled bleeding, visible infection, or trauma that changes appearance or function of the mouth.
Recognizing Dental Emergencies
A true dental emergency affects eating, breathing, speaking, or causes uncontrollable pain. Examples include a knocked-out permanent tooth, severe facial swelling, or a deep laceration to the lip or tongue that won’t stop bleeding.
Patients should note the timing and cause: a knocked-out tooth from a fall needs immediate reimplantation attempts within an hour for best chance of saving it. Severe swelling near the jaw or throat risks airway compromise and requires urgent evaluation. If a dental device (crown, bridge, implant) breaks and causes sharp injury, same-day repair or protection can prevent further damage.
Keep the tooth moist in milk or saline and avoid touching the root. Apply firm pressure to stop bleeding and seek emergency care if bleeding persists beyond 15–20 minutes.
Common Symptoms That Shouldn’t Wait
Severe tooth pain that wakes a patient at night or intensifies over days often signals an infection or abscess. Symptoms like throbbing pain, fever above 100.4°F (38°C), or a bad taste in the mouth suggest pus and spreading infection.
Persistent, spreading facial swelling, difficulty swallowing or breathing, and swollen lymph nodes point to a spreading infection that can become systemic. High fever combined with dental pain needs urgent assessment and probable antibiotics plus drainage.
Sudden loss of a tooth’s fit, new mobility, or severe sensitivity to hot/cold that doesn’t respond to home care should be assessed promptly to avoid worsening damage. Uncontrolled bleeding after an extraction or injury that soaks through gauze requires immediate attention.
When to Seek Immediate Help
Seek immediate help when a tooth is completely displaced, a child has a knocked-out permanent tooth, or there is continuous bleeding for more than 15–20 minutes despite pressure. Also go to emergency care for signs of systemic infection: fever, chills, rapid swelling, or trouble breathing.
If dental pain comes with swelling that pushes the jaw closed or causes drooling, treat it as urgent. Rapid-onset, severe pain after trauma, or any injury that fractures the jaw or causes changes in bite or jaw movement warrants same-day imaging and repair.
Call an emergency dental clinic or visit an urgent care facility with dental services. Bring any broken tooth fragments in milk or saline, a list of current medications, and a trusted contact to assist if sedation or transfer becomes necessary.
Types of Dental Emergencies
Immediate action can relieve pain, reduce infection risk, and preserve teeth. The following sections explain practical steps, likely treatments, and when to seek same‑day care.
Severe Toothache Solutions
A sudden, intense toothache often signals an infection, deep decay, or an abscessed tooth. They should treat pain quickly to prevent spread; he or she should rinse with warm salt water and use over‑the‑counter ibuprofen unless contraindicated, avoiding placing aspirin directly on gums.
Dental clinicians will evaluate with a focused exam and X‑rays, then offer targeted treatments such as root canal therapy to remove infected pulp or extraction if the tooth is nonrestorable. They may prescribe antibiotics when there’s facial swelling, fever, or signs the infection is spreading.
For temporary relief before definitive care, a dentist can place a sedative dressing, adjust occlusion if a bite issue causes pain, and provide prescriptions for pain control. Immediate consultation matters when swelling impairs breathing or swallowing, or when pain does not respond to analgesics within 24 hours.
Handling Broken or Chipped Teeth
Minor chips often need smoothing and a cosmetic repair like dental bonding or a porcelain veneer to restore shape and function. He or she should rinse the mouth, apply cold compresses for swelling, and save broken fragments in milk or saline for the dentist to examine.
More extensive fractures that expose tooth pulp require rapid treatment to prevent infection and pain. Options include pulp capping for small exposures, root canal treatment for deep exposure, and full‑coverage crowns for structural support. If the fracture compromises a restoration, the dentist will remove damaged material and rebuild the tooth using adhesive techniques and durable materials suited to the bite forces in back teeth.
Managing Knocked-Out Teeth
A tooth avulsed by trauma can often be saved if replanted within 60 minutes, and success rates improve the sooner it occurs. He or she should handle the tooth by the crown only, rinse debris with water without scrubbing, and try to reinsert it into the socket if possible; otherwise keep it moist in milk or Hank’s Balanced Salt Solution and seek immediate care.
At the clinic, the dentist will assess socket damage, reposition and splint the tooth for 1–2 weeks (longer for mature teeth in some cases), and prescribe antibiotics and tetanus evaluation as needed. Follow‑up includes monitoring for root resorption and assessing pulp vitality; root canal therapy is commonly performed on mature teeth within 7–14 days to prevent infection.
What to Do Before You Reach the Dentist
Act quickly but calmly. Control bleeding, reduce pain, and preserve any tooth fragments or a knocked-out tooth for possible reattachment.
First Aid Tips for Dental Trauma
Control bleeding by having the patient bite gently on sterile gauze or a clean cloth for 10–20 minutes. If bleeding soaks through, replace the gauze and keep steady pressure; do not remove gauze repeatedly to check the wound.
For lip or cheek cuts, apply a cold pack outside the mouth for 10 minutes on, 10 minutes off to limit swelling. If swelling or severe bleeding persists, seek emergency medical care for evaluation of soft-tissue injury and possible stitches.
Check for signs of concussion after a blow to the head: confusion, nausea, dizziness, or brief loss of consciousness. If any of those are present, take the patient to an emergency room before dental care.
Pain Relief at Home
Rinse the mouth with warm salt water (½ teaspoon salt in 8 ounces of water) to clean the area and reduce bacteria. Use short, gentle rinses and avoid vigorous swishing near loose teeth.
Give over-the-counter pain relievers such as ibuprofen (200–400 mg every 4–6 hours as needed) unless contraindicated; acetaminophen is an alternative for those who cannot take NSAIDs. Follow label dosing and check for allergies or medical restrictions.
Apply a cold compress to the cheek for 10–15 minutes to reduce pain and swelling. Avoid placing aspirin directly on the gums or tooth; topical aspirin can irritate oral tissues.
Preserving Dislodged Teeth
Handle a knocked-out tooth by the crown only; avoid touching the root to protect periodontal cells. If dirty, gently rinse the tooth with milk or saline for no more than 10 seconds—do not scrub or use soap.
If possible, reinsert the tooth into its socket and have the patient bite gently on gauze to hold it in place. If reinsertion isn’t possible, keep the tooth moist by placing it in cold milk or a tooth preservation kit (HBSS). As a last resort, keep it in the patient’s mouth between cheek and gum if they are conscious and can hold it safely.
Transport the tooth and the patient to the dentist within 30–60 minutes for the best chance of reattachment. Contact the dental office en route to alert staff and prepare for immediate treatment.
Modern Approaches to Emergency Dentistry
Modern emergency dental care in Burbank emphasizes fast, accurate diagnosis; patient comfort; and treatments that preserve as much natural tooth structure as possible. Patients can expect digital imaging, targeted pain control, and options that minimize recovery time and future problems.
State-of-the-Art Diagnostic Tools
Clinics use digital X-rays and cone beam computed tomography (CBCT) to pinpoint fractures, root issues, and impacted teeth within minutes. Digital sensors reduce radiation and produce high-resolution images that dentists can view and annotate with patients on a monitor.
Intraoral cameras show close-up views of chips, cracks, and soft-tissue injuries, helping patients understand the findings. Pulp vitality testing and laser fluorescence (DIAGNOdent) detect early decay beneath restorations without invasive probing.
Electronic charting and practice-management software speed triage and coordinate care with other specialists. This tech-driven workflow shortens wait times and improves diagnostic accuracy for urgent cases.
Comfort-Focused Treatments
Emergency teams prioritize immediate pain relief using targeted local anesthesia and short-acting sedatives when necessary. For anxious patients, nitrous oxide or oral sedation provides calm, while monitoring ensures safety during procedures.
Soft-tissue lacerations receive gentle irrigation and absorbable sutures to reduce follow-up visits. For toothaches, pulp therapy or temporary protective restorations relieve sensitivity while planning definitive care.
Clinics stock a range of analgesics and prescribe antibiotics only when indicated, following current antimicrobial stewardship practices. Staff also explain home-care steps—cold compresses, diet adjustments, and pain management—to help patients feel better between visits.
Minimally Invasive Options
When possible, dentists choose conservative repairs: bonded composite fillings for fractured cusps, fiber posts for weakened roots, and onlays instead of full crowns. These approaches conserve enamel and dentin, maintaining tooth strength over time.
For infected teeth, pulpotomy or partial pulpectomy can avoid immediate root canal therapy in select cases, stabilizing the tooth and relieving pain. Extracorporeal splinting or adhesive splints reattach loosened teeth while promoting healing.
When extraction is unavoidable, atraumatic techniques protect bone for faster healing and future implant placement. Clinicians discuss each option’s pros, expected lifespan, and maintenance so patients make informed decisions.
Choosing an Emergency Dentist in Burbank
Finding the right emergency dentist means balancing clinical skill, quick access, and clear communication. Prioritize providers who handle severe pain, broken teeth, and infections efficiently while keeping patient comfort and clear follow-up plans front and center.
Qualities to Look For
Look for dentists with specific emergency experience and up-to-date credentials. Verify state licensure, advanced training in emergency care or oral surgery, and memberships in professional organizations like the American Dental Association.
Clinical competence shows in documented experience treating avulsed teeth, severe infections, and facial trauma. Ask whether the office uses digital X-rays, intraoral cameras, and sedation options to speed diagnosis and reduce discomfort.
Patient-focused traits matter: friendly staff, clear pain-control protocols, bilingual services if needed, and transparent pricing. Read recent patient reviews that mention wait times, pain relief success, and post-procedure follow-up. These practical details predict real-world performance.
Questions to Ask Your Dental Provider
Ask direct, specific questions that reveal readiness and limits. Example questions: “Do you accept walk-ins for dental emergencies?”, “What is your typical wait time for emergency visits?”, and “Which insurance plans and payment options do you accept?”
Probe clinical capabilities: “Can you treat dental infections and perform extractions the same day?”, “Do you refer to oral surgeons for complex trauma?”, and “What pain-control and imaging tools do you use?”
Clarify logistics: “What are your after-hours contact procedures?”, “Will I get a written treatment plan and cost estimate?”, and “How do you handle follow-up care or complications?” Keep answers in writing when possible to avoid confusion later.
Availability and Convenient Access
Prioritize clinics that post real-time hours and offer same-day appointments or clear walk-in policies. Confirm whether the practice provides evenings, weekends, or on-call coverage for nights and holidays.
Check location and parking: choose a clinic within 15–20 minutes of home or work in Burbank on routes with reliable parking or public transit access. This reduces delays when pain or bleeding makes travel difficult.
Verify communication channels: direct phone lines, online booking, and text confirmations streamline emergency response. Also confirm whether the clinic coordinates with local hospitals for severe cases requiring hospital-level care.
Steps to Prevent Dental Emergencies
Preventing dental emergencies focuses on daily habits, protective gear for high-risk activities, and quick attention to small problems before they worsen. These steps reduce the chance of sudden pain, infection, or tooth loss and help maintain long-term oral health.
Healthy Habits for Strong Teeth
Daily brushing with a fluoride toothpaste twice a day removes plaque and strengthens enamel. A soft-bristled toothbrush and 2 minutes per session reach all tooth surfaces; replace the brush every 3 months or after an illness.
Flossing once daily clears debris between teeth where a brush can’t reach, lowering the risk of cavities and gum disease. Using an interdental pick or water flosser helps people with bridges, braces, or limited dexterity.
Limit sugary snacks and acidic drinks like soda and citrus juices; these erode enamel and fuel bacteria. Rinse with water after eating and wait 30 minutes before brushing to avoid brushing softened enamel.
Schedule dental exams and cleanings every 6 months or as the dentist recommends. Professional cleanings remove hardened tartar and allow early detection of cavities or cracks before they become emergencies.
Using Mouthguards for Sports
Wearing a properly fitted mouthguard prevents tooth fractures, loosened teeth, and soft-tissue injuries during contact or high-impact sports. Custom mouthguards made by a dentist fit the mouth precisely, provide better protection, and last longer than boil-and-bite types.
Youth athletes benefit from custom guards because developing jaws change size; a dentist can recommend replacements as needed. For patients with braces, a special orthodontic mouthguard protects both teeth and appliances.
Non-sport activities like biking, skateboarding, or recreational skiing also carry risk; using a mouthguard for any activity with a fall or collision risk is prudent. Store the mouthguard in a ventilated case, clean it after each use, and check for wear—replace when torn or misshapen.
Addressing Minor Issues Early
Small problems such as a chipped tooth, persistent sensitivity, or a loose filling can escalate into infections or tooth loss if untreated. Patients should contact their dental office promptly when they notice changes like a crack, prolonged pain, swelling, or a crown that feels loose.
Interim steps at home include rinsing with warm salt water to reduce bacteria and swelling, and using over-the-counter pain relievers per label instructions for pain control. Avoid chewing on the affected side and keep the area clean.
The dentist can often restore minor damage with composite bonding, replace failing restorations, or prescribe antibiotics when infection is present. Early in-office treatment usually requires less invasive procedures and lowers the chance of emergency visits.
Aftercare and Recovery Tips
Expect clear, specific instructions about pain control, bleeding, diet, and follow-up after emergency dental care. Following those instructions closely helps reduce complications and speeds healing.
What to Expect Post-Treatment
Right after treatment, patients often feel numbness from local anesthesia for 1–4 hours. Mild throbbing or soreness usually peaks 24–48 hours and improves with prescribed or OTC pain relievers such as ibuprofen 400–600 mg every 6–8 hours as directed.
Some bleeding or oozing is normal for 12–24 hours after extractions or surgical procedures. Bite on sterile gauze for 30–45 minutes; if bleeding continues, replace gauze and apply firm pressure for another 30 minutes. Seek immediate care if heavy bleeding soaks a gauze pad in under an hour.
Swelling commonly appears 24–48 hours after trauma or surgery and may last 3–5 days. Apply an ice pack for 10–20 minutes on, 10 minutes off during the first 24 hours, then switch to warm compresses to promote circulation. Fever over 101°F, persistent severe pain, spreading redness, or drainage warrant prompt contact with the dental office.
Caring for Your Mouth at Home
Keep the surgical site clean but avoid vigorous rinsing or spitting for 24 hours to protect forming clots. After 24 hours, rinse gently with warm salt water (½ teaspoon salt in 8 ounces of water) four times daily, especially after meals, to reduce bacteria and debris.
Stick to a soft-food diet for 3–7 days: yogurt, smoothies (use a spoon, not a straw), mashed potatoes, scrambled eggs, and well-cooked pasta work well. Avoid hard, crunchy, sticky, or very hot foods that can dislodge sutures or irritate tissues.
Maintain oral hygiene by brushing teeth gently, avoiding the treated area for the first 24 hours, then cleaning around it carefully with a soft toothbrush. If the dentist prescribed antibiotics or a mouth rinse, finish the full course exactly as directed. Call the clinic if stitches loosen, persistent numbness lasts beyond expected anesthesia, or symptoms worsen.
Why Timely Action Matters
When a tooth is knocked out or a crown comes loose, minutes can change the outcome. Prompt care often preserves the tooth and reduces the need for more invasive treatments later.
Delaying treatment raises the risk of infection and increased pain. Infections can spread to surrounding tissues and may require antibiotics or root canal therapy.
Quick action improves success rates for saving teeth after trauma. For example, replanting a knocked-out tooth within an hour gives the best chance of stabilization and recovery.
Early attention also limits long-term costs and complex procedures. What starts as a simple repair can become a bridge, implant, or extended restorative work if left untreated.
Patients feel more comfortable and recover faster when they seek care promptly. Emergency-focused practices in Burbank prioritize pain control, gentle techniques, and clear explanations to reduce anxiety.
Practical steps help: call the dental office immediately, bring any displaced tooth or fragments in milk or saline, and avoid touching the root. These small actions make a measurable difference in outcomes.
They should contact a local emergency dentist at the first sign of severe pain, swelling, persistent bleeding, or dental trauma. Early consultation guides next steps and preserves oral health.
Gentle Call for Consultation or Questions
They welcome phone calls and messages for urgent concerns or simple questions about symptoms. Staff respond promptly and explain next steps in plain language so patients know what to expect.
If pain, swelling, or a lost filling occurs after hours, they provide clear guidance for immediate home care and arrange the earliest available appointment. Insurance and payment options are explained kindly to reduce stress.
Patients may prefer a quick photo or a brief list of symptoms before the visit; this helps the team prioritize care. They encourage sending details through the office portal or calling directly for faster triage.
For routine follow-up or preventive advice, they offer straightforward tips to avoid repeat emergencies. Simple changes—like timely cleaning and protective night guards—often prevent future problems.
Call the office, use the online form, or send a secure message to ask questions or request a consultation. The team aims to make the process smooth and reassuring so patients feel supported every step of the way.
Frequently Asked Questions
This section answers common urgent dental concerns in Burbank, CA, including what qualifies as a same-day emergency, immediate at-home pain relief, steps after trauma, typical timelines for pain and swelling control, booking options for fast care, and what to bring plus likely costs without insurance.
What counts as a true dental emergency, and when should I be seen the same day?
True dental emergencies include uncontrolled bleeding, severe facial swelling affecting breathing or swallowing, a tooth knocked completely out, and intense tooth pain that prevents sleeping or eating. These situations require same-day evaluation to prevent permanent damage or systemic complications.
Other urgent issues include deep infections with fever, broken teeth causing sharp edges that cut the tongue or cheek, and recent dental work with sudden, severe pain. If symptoms are sudden and severe, contact an emergency dentist immediately.
If I have a severe toothache, what can I do at home to stay comfortable until I get to the dentist?
Rinse the mouth gently with warm salt water to reduce bacteria and soothe tissues. Use over-the-counter pain relievers like ibuprofen or acetaminophen per label instructions, unless contraindicated.
Avoid placing aspirin directly on the gum or tooth. Apply a cold pack to the cheek in 10‑minute intervals to reduce swelling and numb pain.
What should I do right away if I chip, crack, or knock out a tooth?
For a chipped or cracked tooth, rinse with warm water and save any large fragments in milk or saline. Apply a cold compress for swelling and avoid chewing on that side.
If a tooth is completely knocked out, pick it up by the crown, rinse briefly without scrubbing, and try to reinsert it into the socket. If reinsertion isn’t possible, store the tooth in milk or Hank’s Balanced Salt Solution and get to an emergency dentist within 60 minutes for the best chance of saving it.
How quickly can an emergency dentist relieve pain and swelling, and what treatment options might be used?
An emergency dentist can often provide pain relief during the first visit using local anesthesia, short-course antibiotics for infection, and prescription pain medication if needed. Swelling may decrease within 24–72 hours after appropriate treatment begins.
Treatment options include drainage of an abscess, root canal therapy, temporary or permanent dental restorations, tooth extraction, and soft-tissue repair. The specific plan depends on diagnosis and the patient’s medical history.
Do you accept walk-ins or offer after-hours care, and how do I book the fastest appointment?
Many Burbank emergency dental clinics accept walk-ins and maintain extended weekday hours or weekend availability. Call the clinic’s emergency line for the fastest response and to confirm walk-in capacity before heading over.
Some practices use online urgent-care forms or text lines to triage patients quickly. If symptoms threaten breathing or life, call 911 or go to the nearest emergency department.
What should I bring to an urgent visit, and how much might emergency dental care cost if I don’t have insurance?
Bring a photo ID, any dental records or recent X-rays if available, a list of medications and allergies, and the knocked-out tooth in milk or saline if applicable. Also bring a payment method and, if possible, a companion for transportation after sedation or extraction.
Out-of-pocket costs vary: a basic urgent exam often ranges from $75–$200, emergency extractions from $150–$600, and root canal therapy from $700–$1,200 depending on tooth complexity. Clinics may offer payment plans, sliding-fee options, or same-day financing—call ahead to confirm pricing and options.